TRAUMATIC SHOULDER DISLOCATION
What Are the Types/Causes of Shoulder Dislocation?
The shoulder is the most commonly dislocated joint. This is probably because the shoulder is also the most mobile joint in the human body and to achieve this its socket is almost flat and the joint relies on soft tissues such as ligaments and muscles to maintain stability. There are 3 general types/causes of shoulder dislocation: traumatic (most common), atraumatic due to hyperlaxity, and muscle patterning (rare). Some patients may have subtle elements of more than one of these types/causes.
You can learn more about non-traumatic instability here.
Shoulder dislocations due to trauma and injury are most common and of these anterior shoulder dislocation is the most common (90%). Posterior dislocation is a rare form of traumatic dislocation often caused by seizure or electrocution.
In this video we discuss the causes and management of traumatic shoulder dislocations:
What Structures Keep the Shoulder Stable?
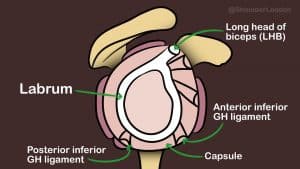
The shoulder joint is the most mobile joint in the body and relies on various structures to keep it stable and prevent it from dislocating. Structures that stabilise the shoulder are divided into static stabilisers (structures that don’t move) and dynamic stabilisers (structures that move). The static stabiliser of the shoulder is the bony structure of the socket. The shoulder can be considered as a golf ball (ball of shoulder or humeral head) balancing on a golf tee (small flat socket). Because the socket of the shoulder (glenoid) is relatively flat it doesnt provide much stability but allows a great range of movement.
In order to deepen the shoulder socket (glenoid) it is surrounded by a rim of tissue called the labrum. Attached to the bottom of the labrum are the anterior and posterior inferior glenohumeral ligaments. These ligaments connect the glenoid (socket) to the humeral head (ball) and are dynamic stabilisation especially when the shoulder is moved into abduction. The inferior glenohumeral ligaments are dynamic stabilisers.
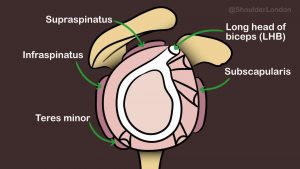
The shoulder also relies on the rotator cuff muscles, subscapularis at front, supraspinatus at the top, infraspinatus and teres minor at the back to provide dynamic stabilisation and keep the ball balanced on the socket.
Damage to the labrum, glenohumeral ligraments, glenoid bone (socket), or rotator cuff, can lead to recurrent instability.
In the video below we explain what happens during an anterior shoulder dislocation:
Do All Shoulder Dislocations Need Surgery?
Some dislocations are unable to be reduced in the emergency department and need an urgent general anaesthetic to put the shoulder back into joint. After this assessments need to be done to determine the cause and severity of the dislocation.
Most atraumatic and muscle patterning dislocations do not require surgery and are best treated with physiotherapy.
Most first time dislocations do not require surgery and they can be managed with physiotherapy, however recurrent dislocations may require surgery to stabilise the shoulder and prevent further damage. The risk of recurrent dislocation after a first time traumatic anterior dislocation depends on age, bony damage, rotator cuff injury.
In patients under the age of 30 with a simple, first time shoulder dislocation, the risk of recurrent dislocation is 90% and this increases to almost 100% if the patient is under 20. In elderly patients recurrent dislocation can occur if there is a massive tear of the rotator cuff muscles. If there is significant bony damage to the socket (glenoid) there may be recurrent instability regardless of age.
What Tests Are Needed to Plan Anterior Shoulder Dislocation Surgery?
After a shoulder dislocation an xray is required to confirm the dislocation and to rule out fractures. After the dislocation is reduced (usually in the emergency department) further xrays are needed to confirm the shoulder is reduced and there are no associated fractures of the ball (humeral head) or socket (glenoid).
In cases of recurrent anterior dislocation, an MRI arthrogram is needed to confirm if any of the stabilising structures are injured. An MRI arthrogram involves a radiologist using ultrasound to put dye into the shoulder with a needle and then the patient is placed into the MRI scanner. We use the dye to see if the ligaments or labrum are separated from the socket.
In cases where there may be fractures or bone loss, a CT scan may also be needed to determine the extent of bone loss in order to plan anterior shoulder dislocation surgery.
Can My Shoulder Be Stabilised With Key-Hole Surgery?
Recurrent anterior dislocations may require surgery but the type of surgery needed depends on whether there is significant bone loss from the recurrent dislocations or whether the injury is purely a soft tissue one.
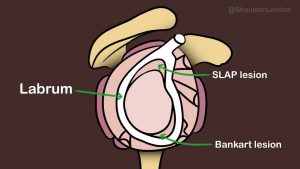
Soft tissue injuries from a traumatic anterior shoulder dislocation include injuries to the anterior inferior labrum (called a Bankart Lesion). When the ball of the shoulder dislocates forward it detaches the labrum from the socket and this causes the anterior inferior glenohumeral ligament to become slack. This can lead to recurrent instability.
One type of anterior shoulder dislocation surgery is an arthroscopic (key-hole) shoulder stabilisation. This can be used to repair the labrum to the socket. Repairing the labrum repairs the tension to the anterior inferior glenohumeral ligament and stabilisises the shoulder.
What is an Arthroscopic Shoulder Stabilisation?
An arthroscopic shoulder stabilisation is a key-hole procedure to repair a labral injury (Bankart lesion) to the shoulder to treat recurrent instability.
In the video below we explain what an arthroscopic stabilisation is:
What Are the Risks of Arthroscopic Shoulder Stabilisation?
It is important that before surgery you understand what is involved in the procedure and what to expect after the surgery. In this video we discuss the procedure of an arthroscopic anterior stabilisation, the post-operative rehabilitation, and risks of the procedure. In clinic prior to deciding on surgery we would discuss any risks that may be specific to you. On the day of surgery we then complete the consent process by discussing these risks again before you sign a consent form.
What Happens if There is Bone Loss to my Socket?
In some traumatic anterior dislocations or cases where there has been many recurrent dislocations, there can be significant loss of bone from the front of the shoulder socket (glenoid). Significant bone loss means the ball of the shoulder has to travel a shorter distance before it dislocates. In these cases the labrum may be significantly damaged and irreparable but simply repairing the ligament would not be enough to prevent further dislocation.
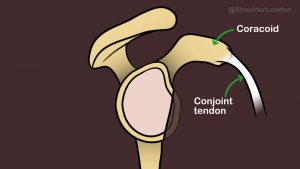
In order to prevent dislocation in these situatons, we use a different form of anterior dislocation surgery operation called an open latarjet stabilisation to restore/increase the width of the socket (glenoid) and prevent further dislocation.
In the video below we explain what an open latarjet stabilisation is:
What is the Recovery From Anterior Shoulder Dislocation Surgery?
The recovery from an arthroscopic shoulder stabilisation and an open latarjet stabilisaiton is the same. Both operations are done as day-case procedures. For both operations we use a sling for 3 weeks. The procedures both require 6 months of physioterapy and contact sport and heavy lifting should be avoided for the first 6 months after surgery.
Our shoulder surgery recovery page gives some indications about how to self care during early recovery. Our post-operative rehab protocol has a table of common post-operative milestones. We have also written a blog about return to driving after shoulder dislocation and shoulder dislocation surgery.
Nick Ferran @ Shoulder & Elbow London Ltd
Clinics in:
Chiswick – Harrow – St. Johns Wood
As an Amazon Associate, I earn from qualifying purchases.